By Stephanie Sugiaman
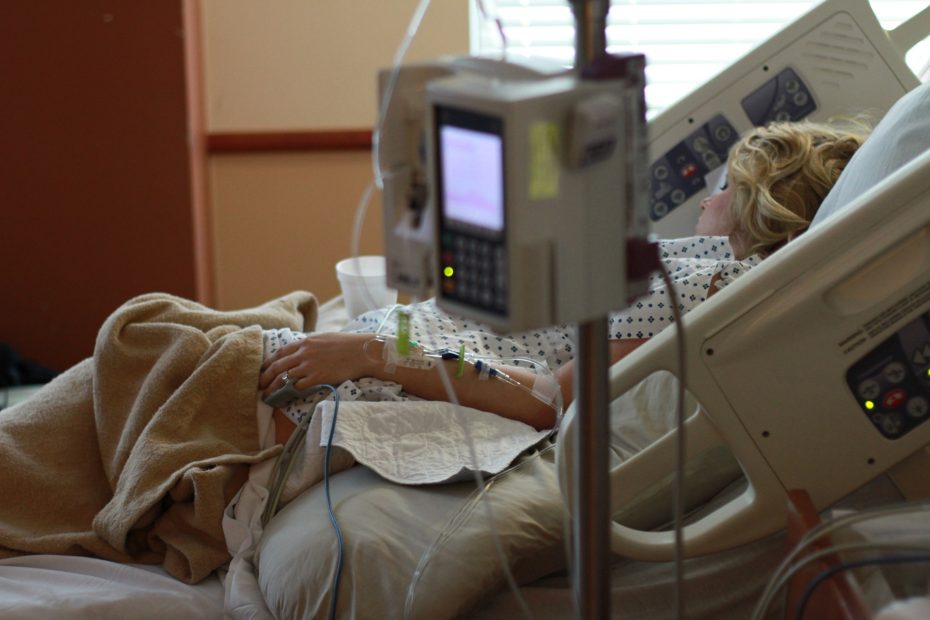
I am a nurse in intensive care in Sydney. We look after a wide range of cases, but mostly respiratory, spinal trauma and burns. I have looked after my fair share of tragic cases, including caring for many palliative care patients. I am no stranger to suffering or death in a hospital setting.
On a personal level, I recently lost my niece and nephew. My nephew’s death was sudden and unexpected; my niece’s death was expected and her battle was long and hard.
I’d like to make a few observations about euthanasia based on my lived experience.
I once looked after a man in his late 70s who had a number of comorbidities, but he was not on death’s door. He came to intensive care for overnight monitoring after a mild procedure.
I received this patient post-op and once I had taken handover from the recovery nurse I went through the usual admission routine of introducing myself, hooking the monitoring equipment up to the patient, and attending to my nursing assessment. Suddenly, he turned and asked me to put him out of his misery.
My first thought was that he must be in a lot of pain — but he told me that he did not have any pain. He explained that he just wanted to be euthanised.
I was quite taken aback, as this man was not seriously ill and would probably go home within the week. I suspected that one of his biggest problems was loneliness.
The state of New South Wales legalised “voluntary assisted dying” a few months ago, although the option will not be available until November 28 next year. So euthanasia was not legal in our hospitals at that stage but my patients was quite insistent. I failed to reassure him and sought help from the medical team and social work.
I also called his next of kin and requested that they visit him. Soon afterwards his three children arrived and spent a few hours with him. The social work team implemented some supportive services to be put into place when he was discharged.
Once everyone had left, I had another conversation with this patient. He was a new man, telling me that he felt happy and didn’t feel like dying anymore. He told me that he hadn’t seen his children in a long time and did not have much support. But after their visit he felt as though this might change.
What does this show?
What we think we desire here and now isn’t necessarily what we need or what is good for us. Our emotions change from minute to minute. If you could change someone’s desire to die into a desire to live, wouldn’t that be worthwhile? If providing love and support meant that a patient gained a few extra years, wouldn’t that be worth aiming for? What we need is more love and more support and less “voluntary assisted dying”.
Another story.
I have cared for a number of patients with traumatic spinal injuries in ICU. These are really devastating. There is a great deal of physical and emotional suffering, including grief over what has been lost. Our patients’ lives have been turned upside down in a blink of an eye. They wake up to learn that they will never walk again. Some will never breathe again without assistance.
But these patients are well supported in Australia. We often see smiling faces coming back in their wheelchairs to thank us and show us the progress they have made since leaving our unit.
I once cared for a seriously injured spinal patient. He was awake and aware of his injuries. He had had a tracheostomy and was supported by a ventilator while a different set of muscles learned to take over his breathing function and while his lungs slowly adjusted to this new way of breathing.
This patient was aware that he would never walk again and that possibly it would take a long time for him to learn to breathe on his own again.
On my shift he became quite distressed. Despite making use of all of our communication methods for this type of patient, I could not work out what he was saying. Nor could the medical team or the speech pathologist. So the medical team decided to let the cuff on the tracheostomy down a bit to allow the patient to speak briefly.
It turned out that he wanted us to euthanise him. But euthanasia was illegal and he was not even a palliative case. I was shaken because his suffering was so palpable and there was little I could do to ease it.
But he had a loving wife and two young children. He progressed through ICU and went first to the spinal unit and then to spinal rehabilitation. A few months later we received a testimony from him; he told us how much he had to live for. He was still able to enjoy his family life and professional career, and even some long-term hobbies.
How beautiful it is to witness someone struggle through a life-changing ordeal and emerge happy and content. If “voluntary assisted dying” had been an option in my workplace at the time, this man would have died. If he didn’t have a loving family, he might have died.
Suffering has value
You might tell me: you’re a nurse; you’re too detached from the suffering your patients go through. This is true, of course, although professional detachment is important.
But as I watched my niece Ellie die of a brain tumour, I came to understand why people might think that euthanasia is a good idea. As a nurse I have to maintain a professional distance, but I felt my niece’s suffering on a personal level. It was extreme, and I say this an intensive care nurse who has witnessed more illness and suffering than the average person. I understand how relatives might feel that euthanasia is a good option.
But I also grew to understand the value of personal suffering; it showed me that it is worth fighting to the end and allowing nature to take its course.
In her final months Ellie could no longer walk and could only leave her bed to sit down with the assistance of equipment and a lot of hard work.
In her final weeks she could no longer speak. Her ability to eat declined. She was hungry but she simply couldn’t eat.
In her final days, her only form of communication was the movement of her eyeballs up and down, at best. A movement meant Yes; no movement meant No.
So Ellie’s slow death was more brutal than most people experience. But she was constantly surrounded by love. Twenty-four hours, day and night, my sister, my brother-in-law, my mother and other nieces were with her.
She had many visitors and even though she could not speak, she was able to give people a smile, often a laugh. My young son and my nephew were amongst those who gave her the most joy, also showing what a gift children can be. Her smile was infectious and showed us how someone can choose to live with joy and happiness in the midst of difficulty and suffering.
My sister, my nieces, and I washed her when she became helpless; what a privilege it is to be trusted with something so vulnerable! Our hands became a gift to Ellie, bringing her comfort and dignity in the last stages of her life and giving her the opportunity to say Yes to vulnerability and true love. And Ellie became a gift to us all in so many ways.
Love allows people to thrive; love carries people through the most difficult moments of suffering. Without that love — who knows? — maybe Ellie too would have desired euthanasia.
Being given the opportunity to love someone through their suffering is a privilege. It permits personal growth that may not have happened otherwise.
Perhaps some readers might say that I’m talking too much from my own perspective and not from Ellie’s. But I can assure you that she would never have wanted euthanasia. Why? I would say that it had a lot to do with the love that surrounded her.
That’s why I wonder if those who ask for euthanasia do so because of a lack of love in their lives.
Does our society need to shift its gaze from a quick euthanasia fix towards the long, slow labour of accompanying those who suffer? Human suffering is a part of life, and isn’t life worth living to the full and to the end? Isn’t each individual person worthy of having a life lived and ended well?
To some a “good death” is euthanasia. But to these people I would say: your suffering until the natural end to your life is your gift to those who love you. And their time, work and love are a gift to you.
There are moments of positive transformation for all of us at the end of life. “Voluntary assisted dying” steals those gifts from us.
This article has been reprinted with permission and can be found at mercatornet.com/its-not-too-much-pain-but-too-little-love-that-makes-people-ask-for-euthanasia/81250.